In 2026, Remote Patient Monitoring is no longer optional for US healthcare providers. It has become a core pillar of modern healthcare delivery.
Remote Patient Monitoring (RPM) is now a standard part of care delivery. It allows providers to track patient health in real time. With connected devices, care extends beyond the walls of the practice into patients’ everyday lives.
Through a remote patient monitoring system, providers can collect physiological data such as blood pressure, heart rate, oxygen levels, blood glucose, weight, etc.
Healthcare providers like you are increasingly realizing that traditional in-person care alone cannot meet the growing demand for chronic disease management. Instead, many providers now rely on remote patient monitoring to deliver continuous care and stay connected with patients between visits.
RPM highlights a fundamental shift in how care is delivered, moving from a reactive model to a proactive model. This real-time monitoring allows providers to intervene early, reduce hospitalizations, and improve long-term patient outcomes.
At this point, you may be wondering how RPM works and what devices are used.
Now that you understand the definition and importance of RPM, the next logical question is, ‘How does it actually work in a real clinical setting?’
Let’s explore how remote patient monitoring works in real clinical environments.
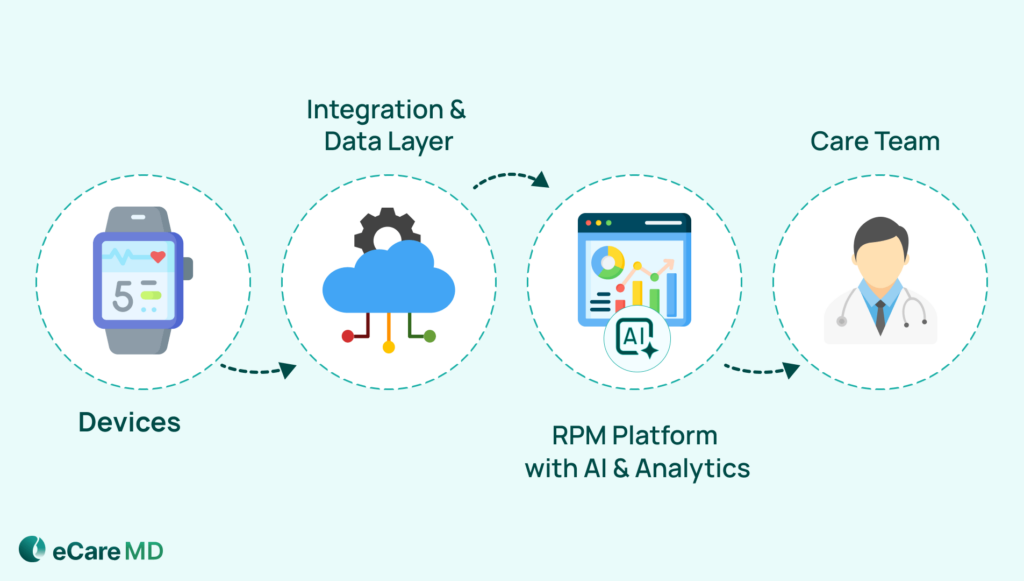
RPM follows a four-step workflow: data collection, transmission, analysis, and clinical intervention. These steps keep patient care connected even outside the clinic walls.
Effective remote monitoring starts with planning, not just data collection, and it begins with identifying the right patients. Individuals with chronic conditions like hypertension, diabetes, or heart failure, or those recently discharged who need closer follow-up, are eligible patients. Providers generally flag these eligible patients during visits, discharge planning, or population health reviews.
The enrollment process begins once a patient is identified. This process includes obtaining consent, verifying insurance coverage (especially for Medicare RPM programs), and documenting eligibility.
After completion of the enrollment process, the next step is patient onboarding, in which patients are introduced to the RPM program, educated on what to expect, and prepared for using monitoring devices effectively.
The next crucial part is device assignment and setup. Patients are either provided with devices in the clinic or have them shipped to their home. These devices depend on their condition. For example, blood pressure monitors, glucometers, pulse oximeters, or weight scales.
Providing a device is not enough; patient engagement is critical for RPM success. It is necessary to educate your patients about how and when to take readings, what to expect, and why consistent monitoring matters.
For example, a patient with hypertension should be instructed to check blood pressure daily at the same time and avoid caffeine beforehand to ensure accurate readings.
Once set up, data collection becomes part of a patient’s daily routine. Readings are captured through connected devices and automatically transmitted to the RPM platform, usually via cellular networks or Bluetooth. This seamless data integration makes RPM easy to scale in high-volume environments.
This stage involves the first two steps of the RPM workflow, i.e., data collection and data transmission. In these steps, patient health metrics are captured and securely transferred through a remote patient monitoring system without requiring in-person visits.
On your side, this data is continuously organized, trended, and filtered through alert systems. This is how clinicians monitor patients remotely using alerts and dashboards. For example, if your heart failure patient shows a sudden weight gain over a shorter period, the system flags it as a potential sign of fluid retention.
Behind the scenes, advanced clinical dashboards and AI-driven analytics help you to focus only on high-risk patients by analyzing incoming data, identifying trends, and flagging abnormalities.
This is also how doctors monitor patients remotely in day-to-day clinical practice. Rather than just reviewing patient data, your care team can respond in real-time. Care coordinators monitor alerts, reach out to patients when needed, and escalate concerns to you for clinical decisions. Based on the situation, you may adjust medications, guide the patient, or schedule a follow-up visit.
In a typical RPM workflow, this is a coordinated team effort. For example, providers make clinical decisions, care coordinators handle patient communication, clinical staff review trends, and patients actively participate by continuously recording their data.
This ongoing process assists you in detecting potential issues earlier and managing patient health more proactively, without relying on frequent in-office visits.
The table below summarizes the RPM workflow:
RPM is often associated with connected medical devices, but it is much more than hardware, but RPM is much more than hardware. These devices are just one key layer of a whole RPM ecosystem to collect patient data.
In reality, RPM is a complete healthcare system that combines devices, software, and connectivity to support continuous care beyond traditional clinical settings.
The real value of RPM lies in its software platforms that collect, organize, and analyze patient health data in one centralized dashboard. Rather than reviewing data from various sources, all patient readings are aggregated into a single view, providing a complete picture of patient health.
Furthermore, you can also analyze the data by identifying trends, comparing readings over time, and flagging any abnormalities. Also, you can quickly detect changes in a patient’s condition through visualizations like charts and graphs.
This allows you to track progress, detect potential issues early, and make informed clinical decisions easily.
The effectiveness of this ecosystem begins with the right devices. Common RPM devices include blood pressure monitors, glucose meters, pulse oximeters, and weight scales. Each device is specifically designed for capturing condition-specific health data for clinical decision-making.
However, not all devices have the same clinical value level. It is also necessary to distinguish medical-grade RPM devices from consumer wearables. Unlike fitness trackers, clinical-grade devices are more accurate and reliable, so the data can be used for real patient care decisions.
Equally important is connectivity. RPM devices usually use cellular (LTE) or Bluetooth connectivity. Cellular devices automatically transmit data, which makes them ideal for elderly or less tech-savvy patients; on the other hand, Bluetooth devices need smartphone pairing, which makes them more suitable for digitally comfortable users.
Device selection is a critical thing as it directly impacts your program’s success. Easy-to-use devices enhance patient adherence, while reliable data transmission ensures timely and accurate clinical insights.
Now that we’ve discussed how remote patient monitoring works and the technology behind it, a common question that you might have is what conditions can be monitored with remote patient monitoring?
RPM is more beneficial for patients with chronic conditions and high-risk individuals who need consistent monitoring. Rather than depending on episodic in-person visits, RPM allows you ongoing visibility into your patients’ health status. This helps you stay ahead of potential complications.
Remote patient monitoring is ideal for chronic diseases, as these types of diseases require continuous data collection. Some of the most commonly monitored conditions include hypertension, diabetes, congestive heart failure (CHF), chronic obstructive pulmonary disease (COPD), and asthma.
Let’s have a quick look at the most widely monitored conditions:
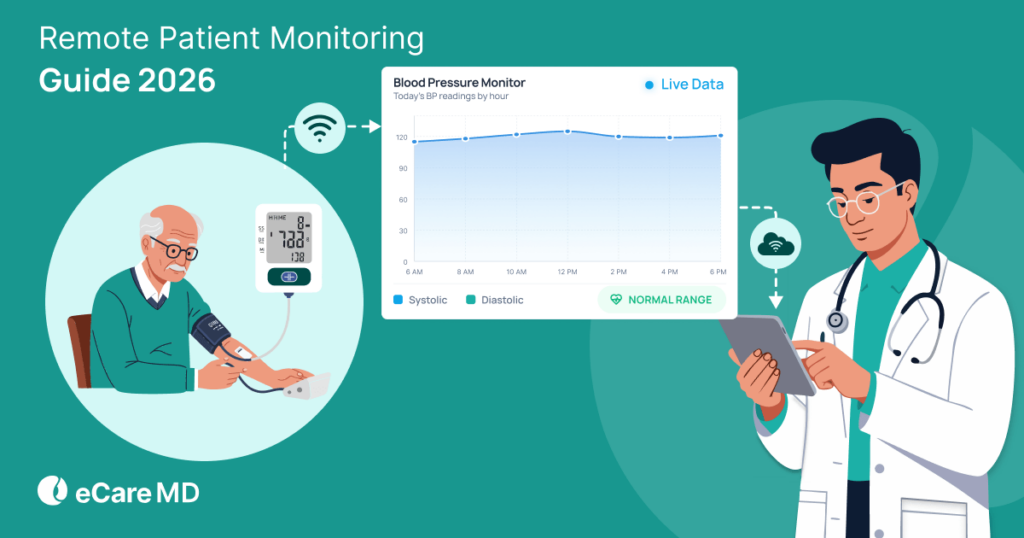
For your better understanding, let’s take one example. Patients with hypertension can regularly check their blood pressure at home using a connected blood pressure monitor. The readings are then automatically transmitted to your monitoring platform, allowing you to track patterns and adjust treatment plans when necessary.
In real clinical settings, it means that there is no need to wait weeks for a follow-up visit to identify a problem. If your patient’s reading starts trending upward, your care team can take quick action by adjusting medications, providing guidance, or scheduling a timely consultation.
While RPM supports many conditions, not every patient can automatically enroll in an RPM program. This raises an important question: who qualifies for RPM programs?
Medicare patients with acute or chronic conditions who require regular physiological data collection are usually eligible for RPM programs. Furthermore, patients with two or more chronic conditions or recent hospital discharges are also eligible for the RPM program. However, eligibility criteria continue to evolve with CMS policy updates.
RPM is transforming chronic disease management from reactive to proactive, continuous care. From this approach, you can be continuously informed about your patients’ health, instead of only seeing snapshots during appointments.
As the healthcare industry is moving towards value-based care models, remote patient monitoring is becoming an increasingly valuable tool for both healthcare providers and payers. Along with clinical applications, RPM also provides significant operational and financial advantages.
RPM is not just a monitoring tool, it is a care transformation strategy that can enhance outcomes and reduce avoidable healthcare utilization.
Reducing hospital readmissions by intervening early, new CMS reimbursement revenue, enhancing chronic disease outcomes, and greater operational efficiency are some of the major benefits of remote patient monitoring to providers.
One of the key advantages of RPM is enhancing clinical outcomes, driven by continuous and data-based monitoring. This helps you to make timely and informed decisions.
Early detection of health deterioration is another key benefit. As RPM enables you to track your patient data continuously, you can easily identify subtle changes early. This proactive approach can help you to prevent complications and reduce emergency interventions.
Additionally, RPM also supports population health strategies by allowing proactive management of the highest-risk patients. RPM shifts care from expensive acute interventions to lower-cost preventive monitoring. On top of that, RPM can improve care coordination across multi-provider care teams.
Beyond providers’ benefits, RPM also enhances patient satisfaction by providing a connected and proactive care experience, continuously supporting patients.
Together, all these pointers make the RPM program an important component of the modern healthcare delivery models.
To explore more about how RPM contributes to value-based care, you can explore our guide: How Remote Patient Monitoring Supports Value-Based Care for Medicare Providers.
While the RPM offers significant clinical and operational benefits, implementing it comes with a lot of challenges. The transformation from the traditional care model to remote patient monitoring requires workflow adjustments, staff training, and the integration of new technologies into existing systems.
When practices are shifting from episodic care to continuous care, these challenges are common during the initial phase.
One of the biggest implementation challenges is adjusting existing clinical workflows. As mentioned previously, RPM collects continuous patient data; if this data is not routed through the correct person, it creates obstacles like delayed clinical response and workflow inefficiencies. An easy solution for these challenges is to exactly define how alerts are classified and who will respond.
That’s why, before implementing, clear workflow mapping is important. Defining escalation paths, assigning responsibilities, and setting response timelines ensures that no alert is missed or delayed.
The next critical challenge you may face is staff adoption, which requires deliberate change management. You have to train your care team constantly, not just a one-time event. Along with this, it is important for your care team to understand the clinical value of the program.
Additionally, before patient onboarding begins, proper provider training is important. It helps you to ensure that your clinical staff is confident in using the system and responding effectively to patient data. Without this foundation, even the best RPM tools can fail.
Furthermore, another real risk is data overload. Your care team can definitely be overwhelmed by large volumes of readings. To overcome this, well-designed RPM systems and monitoring protocols are essential.
You can prevent data overloading by focusing on actionable insights instead of raw data. You can achieve this through automated alerts, predefined thresholds, and intelligent filtering, as all these features highlight clinically relevant changes.
Rather than relying on manual review of patient data, you can rely on automated alerts, predefined thresholds, and intelligent data filtering.
Rather than launching RPM for all patients at once, starting it with a defined patient population is another key practice. If you start with high-risk or chronic patients, it can enable you and your care team to refine workflows, enhance efficiency, and build confidence before scaling your program gradually.
Want to launch an RPM program in your practice? Click here to get more information about 5 Best Practices for Starting a Remote Patient Monitoring Program in Your Practice.
To launch a successful remote patient monitoring (RPM) program, it is important to follow a structured, step-by-step approach that goes beyond simply adopting new technology. It requires careful planning across clinical, operational, and technical areas to ensure long-term success.
A well-planned RPM rollout typically includes the following key steps:
The first step is the identification of high-risk patients, such as patients with chronic conditions like hypertension, diabetes, or heart failure. Along with this, defining clear monitoring platforms like tracking vitals, measurement frequency, or alert thresholds is also important to ensure continuous care delivery.
The next step includes the selection of clinical-grade RPM devices that match your patient’s conditions. These devices include blood pressure monitors, glucose meters, pulse oximeters, weight scales, etc. Additionally, this step involves ensuring usability while maintaining clinical accuracy and reliability.
Choosing a platform that integrates seamlessly with your existing healthcare systems is the next step. Your platform should act as an extension of your clinical workflow. Some key factors to consider in this step include EHR integration, scalability, secure data management, and real-time reporting capabilities.
Next, you should define clear responsibilities for your nurses, care providers, and coordinators. You should establish structured escalation protocols to ensure every alert has a defined response pathway. This assists you in reducing delays and ensuring timely clinical intervention when patient data signals risk.
Along with all these, the next important step is to educate your patients on how to use RPM devices, when to take readings, and why consistency matters the most.