The traditional fee-for-service payment model indeed helped healthcare providers incentivize their services, but the patient outcomes fell short of expectations. This demanded a change in the system and a holistic approach to treatment.
This shift led to the rise of value-based care, which not only focuses on evidence-based practices but also enhances the healthcare system by focusing more on patient outcomes and patient satisfaction levels.
But indeed, the benefits of RPM for value-based care have been exceptional, making them a perfect match.
Building on this shift, AI and machine learning are now transforming raw RPM data into actionable quality measures for CMS reporting. This ensures you enhance health outcomes while reducing costs.
But is implementing RPM for value-based care challenging? What are the challenges of using RPM within value-based care?
The answer often depends on how well the implementation process is understood and executed.
So, by simplifying this process, let this blog be your step-by-step guide to implementing value-based care with RPM in your practice.
Before getting into the implementation process, let’s first understand what value-based payment in healthcare is and why it is so important for the future of the healthcare industry.
Traditionally, the payment model followed by the healthcare providers was fee-for-service. Which means that healthcare providers were paid for the service they provided.
For example, if a patient consults a physician for gastroesophageal reflux disease, the patient has to pay the doctor the consultation fees, regardless of the value it brought to the patient.
However, as healthcare shifted toward data-driven and evidence-based practices, this model began to reveal its limitations, particularly its lack of focus on patient outcomes and long-term value.
This volume-driven approach highlights the limitations of fee-for-service. For example, fee-for-service focuses more on quantity than on patient outcomes and satisfaction.
To navigate a way to overcome this, CMS introduced value-based reimbursement, which not only focused on value-based care but also aimed to hold providers accountable for improving patient outcomes.
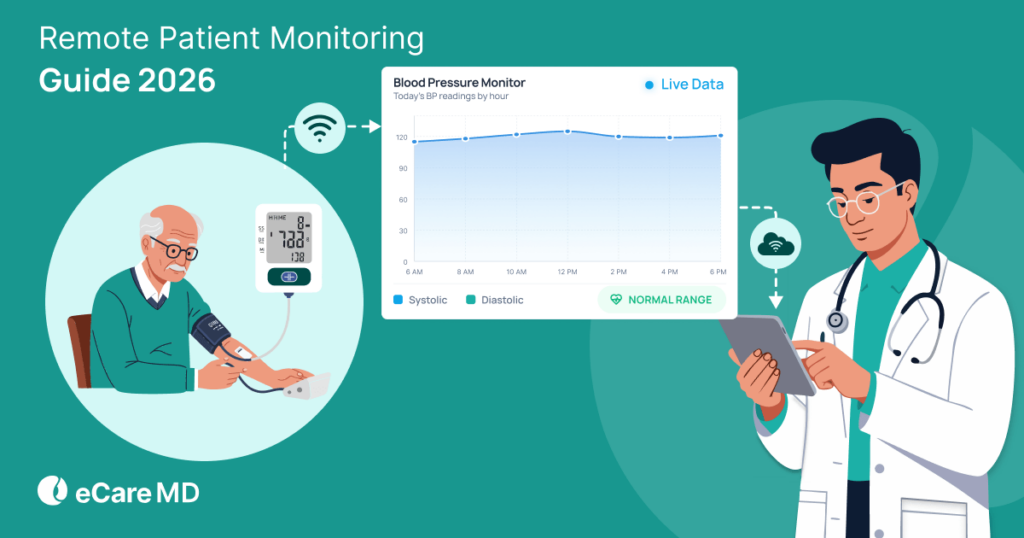
Remote monitoring is now vital for quality, outcome-driven care. It allows doctors to keep a constant eye on patients from afar, helping them make better treatment decisions. Holding patient data as the key indicator in the program strengthens the link between RPM insights and improved outcomes, emphasizing quality of care and patient satisfaction.
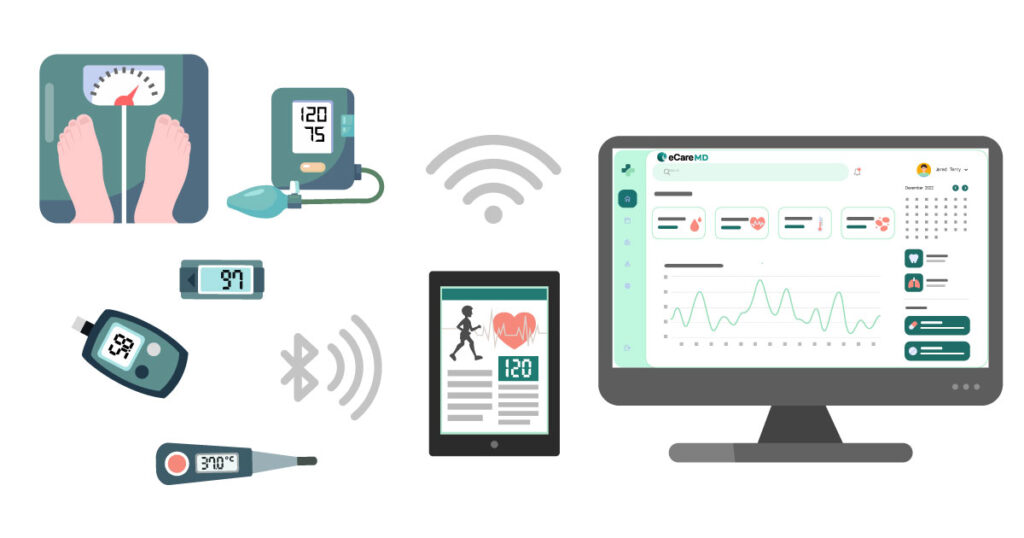
In a nutshell, remote patient monitoring is a way to monitor a patient’s condition and the outcomes of typical healthcare practices. With this, gathering crucial patient vitals in real-time, like blood pressure, heart rate, glucose levels, etc., becomes much easier.
Remote patient monitoring boosted the transition from traditional practices to the digital landscape. Furthermore, the continuous access to patient data in real-time and AI-powered insights transforming it into actionable information allowed providers to make informed decisions, enhancing different aspects of care.
The introduction of RPM drove data-based practices in healthcare and provided a perfect opportunity to boost value-based care models. The integration of RPM allowed providers to have a holistic approach to their care practices, and adapting to the new value-based payment model became much easier.
The most significant benefit of integrating RPM with value-based care has been the change in focus for providers. It gave providers a proactive approach to providing care supported by real-time access to patient data. This not only helped providers in curating personalized care plans but also enhanced preventive care for patients.
By tracking real-time patient data, modern RPM provides continuous health insights. This helps you take a more proactive and preventive approach to care. Additionally, it supports outcome-based care models and aligns with reimbursement programs like Medicare RPM, making value-based care easier to manage and measure.
The major USP of remote patient monitoring is that it directly instills data-based decision-making into your healthcare practice. This enhances chronic disease management, where value-based care contributes to increasing clinical efficiency with RPM.
For your better understanding, let’s explore how RPM supports chronic disease management in practice.
The patients enrolled in your program are assigned particular RPM devices to enable continuous monitoring of patient health. Here, healthcare providers monitor vital biometric data like blood pressure, glucose levels, heartbeats, etc., which equips them with crucial insights for developing an effective care plan.
This continuous monitoring plays a vital role in remote patient monitoring for chronic care management, especially for conditions requiring consistent tracking, such as hypertension, diabetes, and heart disease.
Along with that, data-backed practices change the nature of services being provided from reactive to proactive, where active interventions are enabled. The collected data also acts as a cornerstone for early detection of depleting health conditions, which can be intervened on by care providers to improve patient outcomes.
With AI-enabled trend analysis, you can identify rising-risk patients early and intervene before they reach a complication point. Here, the cost-effectiveness of RPM can be seen in the reduction of hospital readmissions and improved health outcomes for patients.
Furthermore, automated alerts and continuous monitoring support the reduction of hospital readmission through RPM and value-based care protocols, while improving care coordination and overall cost control.
This proactive, data-driven care not only improves patient outcomes but also aligns with value-based reimbursement metrics, supporting financial sustainability.
Along with improving clinical outcomes, RPM also plays a key role in enhancing performance under value-based reimbursement programs.
For Medicare providers, successful value-based care heavily relies on performance under various programs. For example, the Merit-based Incentive Payment System (MIPS) in which remote patient monitoring for value-based care supports both quality and improvement activity categories.
As mentioned earlier, with structured RPM data, you can easily track patient outcomes, document care delivery, and demonstrate measurable improvements in clinical performance.
Additionally, by automating the collection of required G-codes and supporting documentation, RPM can simplify the administrative burden linked to Medicare RPM reimbursement. This is beneficial for providers participating in Medicare Advantage plans and Accountable Care Organizations (ACOs).
Another key advantage is the ability to close gaps in care. Through continuous monitoring and regular patient engagement, RPM helps you to create ongoing touchpoints without requiring frequent in-office visits.
By ensuring timely intervention and consistent care delivery, this improves patient adherence along with outcomes and also supports you to improve MIPS scores with remote patient monitoring.
One of the benefits of RPM in value-based models is that it encourages patients to participate actively in their healthcare journey. Since the patients use RPM devices to collect their health vitals, they can not only self-monitor their health but also actively participate in their care journey by adhering to the care and treatment plans.
Remote patient monitoring for value-based care helps you to improve awareness and strengthen patient involvement by allowing patients to access their own health data and insights.
Along with that, the educational resource library available in the application empowers them with enough information to make necessary changes in their lifestyles. Advanced RPM platforms also integrated digital nudges and AI-driven educational modules to enhance treatment adherence and positive health behaviors.
Furthermore, you can also implement feedback mechanisms to empower patients and alter your care delivery process to improve patient outcomes. When your patients stay informed and engaged, they are more likely to make healthier choices, which ultimately leads to better long-term outcomes in chronic care.
While patient engagement is critical, operational efficiency is equally important for scaling value-based care programs. By automating most of the clinical process, RPM maximizes clinical efficiency and allows healthcare providers to focus on preventive care and make informed decisions by streamlining data collection and analysis processes.
You can easily eliminate data silos and ensure seamless information sharing across systems by integrating RPM for value-based care into clinical workflows through bi-directional EHR synchronization.
Furthermore, the continuous monitoring feature that allows clinicians to intervene in the care procedure significantly reduces the chances of hospital readmission and emergency room visits. This allows better clinic management and improves its efficiency to maximum capacity, further enhancing the practice and adding value to the care being delivered.
AI-driven risk segmentation further enhances population health scalability by grouping patients into low, medium, and high-risk groups, which enables you to optimize resource allocation and targeted care delivery.
Additionally, real-time alerts triggered by abnormal readings allow you to make timely interventions while improving care coordination across clinical teams.
As mentioned earlier, RPM and value-based care are a match made in heaven because of their alignment of the factors or quality metrics. Meaning that the quality metrics used in value-based reimbursement are the same as those used for measuring the success rate of remote patient monitoring programs.
For example, value-based reimbursement considers reduced hospital readmissions, patient engagement levels, medication adherence, improved patient outcomes, etc. These same metrics are used to quantify RPM.
This alignment helps you to prove the value of your value-based contracts with hard data, such as reduced ER utilization and enhanced clinical outcomes, strengthening the case for remote patient monitoring for value-based care.
Along with that, the data generated by RPM devices serves as evidence to deliver care. This way, healthcare providers can accurately diagnose and curate care plans. Furthermore, with continuous monitoring, they can proactively intervene and provide care to improve healthcare outcomes. This way, RPM supports care in value-based contracts.
However, one thing to remember here is to accurately document RPM activities to maximize reimbursement with RPM. Implementation of automated time-tracking and documentation tools helps you ensure audit-proof Medicare RPM reimbursement and supports accurate remote patient monitoring reimbursement.
Furthermore, you can also maximize per-member-per-month (PMPM) revenue by combining RPM with Chronic Care Management (CCM) programs. This further strengthens financial sustainability.