Currently standing at an estimation of $14 billion, do you also think RPM is the future of healthcare?
Setting the Foundation for Success
1. Define Your Patient Population with Data Precision
Furthermore, you can use your EHR or clinical data to identify high-risk patients to make your approach more data-driven. These patients include frequent ER visits, uncontrolled vitals, or poor adherence. These patients are more likely to benefit from remote patient monitoring best practices and deliver a higher return on investment.
Depending on the patient population and the service you will be providing, you need to customize your remote patient monitoring software and workflows accordingly. Address your specialty, specific conditions, and demographics accordingly to add value to your practice.
Along with that, since you will be starting a remote monitoring program, you need to develop a clear value proposition that highlights the benefits for both patients and healthcare providers.
For example, a well-structured RPM program helps you to reduce white coat syndrome and provides a more accurate, continuous, and 360-degree view of your patient’s health outside the clinical setting.
This will help you get a clear picture of your offerings through the program and outline your practice’s workflow accordingly.
Additionally, to select the right patients and maintain standardized care protocols, ensuring alignment with established remote patient monitoring program guidelines is crucial.
Download the Free Guide to Selecting the Right Patients for Your RPM Program
Download Guide2. Implement a "Workflow-First" Tech Strategy
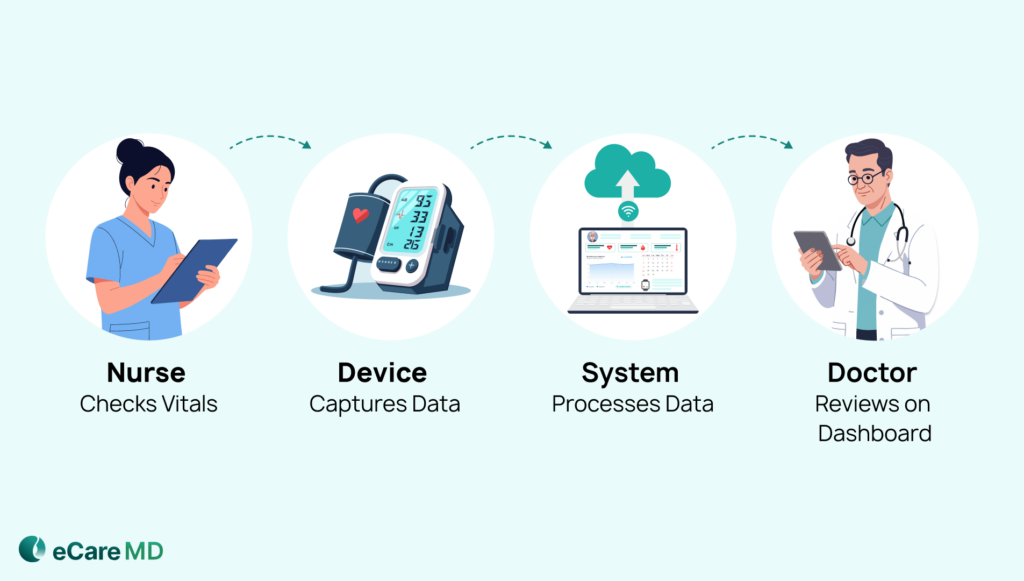
You won’t be treating all of the conditions, so limiting yourself to specific specialties can be healthy for the start of your business. However, selecting appropriate technology can be useful in device selection and creating an ecosystem for its sustenance. Also, choose FDA-approved devices so that they won’t cause legal or regulatory issues.
With eCareMD, you can incorporate AI-driven capabilities into your platform, which will help you filter out irrelevant data. Moreover, it also ensures that your staff focuses only on clinically significant alerts.
With regard to the remote patient monitoring software, prioritize a user-friendly interface and ensure interoperability to streamline data collection and analysis.
For the purpose of improving patient participation, you need a very simple interface for patients who aren’t tech-savvy. By using cellular-enabled, plug-and-play devices, you can make remote monitoring easier for clinics and patients alike.
Along with that, provide effective hands-on training and support to the staff and patients to ensure effective use of monitoring tools and software.
To manage a growing RPM program without increasing staff workload, it is necessary for you to design workflows that are simple, standardized, and scalable.
3. Automate Compliance & Documentation

For better compliance, use the secure remote patient monitoring system to document all patient interactions, alerts, and data transmissions. This also helps you to stay audit-ready and reduces compliance risks.
Along with that, establish clear policies and procedures for data privacy and breach response to gain patients’ and stakeholders’ trust.
Additionally, by using automation tools for documentation and compliance workflows, you can streamline operations, along with ensuring accuracy and consistency in remote patient monitoring.
Register for a Free Webinar on RPM Compliance & Documentation
Register Now4. Design Scalable Clinical Workflows
The key RPM program best practices help you to improve efficiency and allow your single care coordinator to manage a larger patient population efficiently. For example, one of the key best practices for remote patient monitoring programs is the adoption of an exception-based monitoring approach, which allows your care team to intervene only when the system flags abnormal readings.
Furthermore, since both your patients and staff will be using telehealth platforms integrated within the software, provide the users with effective training on how to use the communication tools. This will improve the efficiency of your healthcare practice and reduce the care delivery time.
In addition, your remote patient monitoring system should integrate with your existing EHR systems to enable bi-directional data flow. This will further ensure that RPM insights are directly reflected in the patient’s primary medical record.
At the same time, your workflows should be standardized yet flexible to support various specialties and patient needs. This is essential for scaling remote patient monitoring for clinics.
5. Align Reimbursement with Clinical Outcomes

Start Your Remote Patient Monitoring Program
Conclusion
To start an RPM program, an understanding of the business and the ecosystem it requires is necessary. A healthcare provider can ensure seamless care delivery, but often overlooks the technology part of the process. Some of the important things here are RPM software and its integration with the healthcare systems for the smooth functioning of further operations.
We at eCareMD specialize in that and help RPM businesses build the perfect nervous system for their business. Along with intensive training and access to learning resources, we equip your healthcare practices with all the necessary technology tools for streamlining your RPM services with software.
As discussed above, following the right RPM program guidelines, from defining the patient population to ensuring compliance and aligning reimbursement, is critical for a successful launch.
But this is just one part of setting up the business. The rest of the above section can serve as your guide to the successful development and implementation of your RPM business. So, tickle your entrepreneurial mind and add value to your healthcare practices with strategic business planning.
Click here to know more about it.