Even after implementing RPM, many practices fail to unlock its full potential. This is often due to challenges in meeting Medicare RPM reimbursement requirements.
Major reasons include inefficient workflows, missed clinical time, and reliance on manual processes. The real challenge is translating RPM into consistent revenue. When your teams depend on spreadsheets or disconnected systems, it becomes complex for them to accurately track every interaction.
As a result, even the most valuable clinical time can go unrecorded, leading to underbilling. This is where more advanced RPM reimbursement strategies become necessary. With AI-driven automation, you can reduce human errors, enhance accuracy, streamline workflows, and ensure consistent, compliant documentation.
And this is where you begin to see what your RPM program is really capturing and what it’s not.
So, are you actually capturing all the billable time your team is already putting in?
That’s exactly what we’ll answer in this blog.
Let this blog be your guide to know how to increase remote patient monitoring revenue by using practical strategies and smart processes.
Optimize Patient Onboarding & Device Adherence
The success of your RPM program depends on patient onboarding and their engagement with the devices. Many providers focus on coding but overlook proper device education, which can limit their ability to maximize RPM reimbursement.
This is critical, especially during the initial setup phase of CPT 99453. At this stage, proper training is necessary to ensure that your patients understand how to use their devices accurately and why consistency matters.
When your patients are confident, they are more likely to stay engaged, supporting better remote patient monitoring reimbursement.
Ongoing adherence is also critical to meet the 16-day CPT 99454 requirement. Missing this threshold can cause missed billing opportunities.
To overcome this, many providers are using cellular-enabled, plug-and-play devices that can simplify usage while reducing technical barriers for your patients. This approach helps to maintain eligibility for Medicare RPM reimbursement.
However, consistency can still drop over time, even after using the right devices. This makes smarter RPM reimbursement strategies an important factor. AI-driven systems can help you send automatic reminders to patients who are at risk of missing their required readings. This ensures that they stay on track without adding extra staff workload.
At the same time, initial education also assists you in the reduction of future support needs while preventing patient drop-offs. Your patients are more likely to engage when they clearly understand the process from day one.
By understanding all these factors, you might have realized that patient adherence directly impacts your ability to maintain consistent billing cycles. Strong onboarding and continuous engagement enhance outcomes and strengthen your remote patient monitoring reimbursement and overall RPM billing optimization.
Mastering the Clinical Time-Tracking Workflow
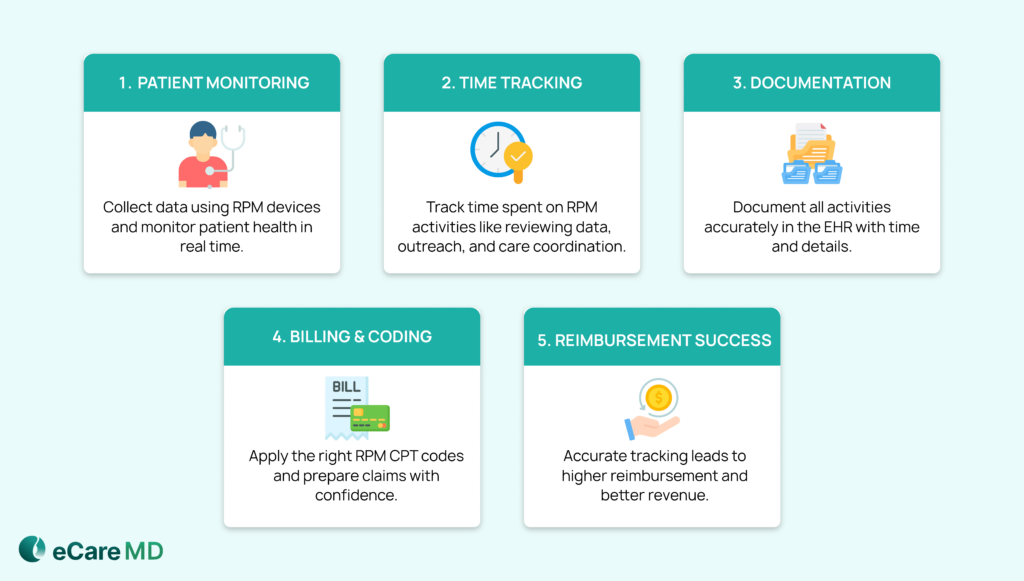
After patient onboarding and adherence, the next question is: ‘How to ensure that every minute of care delivered is accurately captured?’ Without a reliable system, it’s difficult to maximize RPM reimbursement, even if your team is actively managing patients.
Many practices still depend on manual methods for tracking the required 20 minutes of clinical time. But this approach can lead you to miss activities, which can directly affect remote patient monitoring reimbursement.
To avoid this issue, you need more structured and consistent workflows. This is necessary especially when optimizing RPM clinical time-tracking for 99457, where every interaction, like reviewing patient data or adjusting care plan, must be properly recorded.
When workflows are clearly defined, it’s easy for your care teams to capture all eligible activities without relying on memory or any scattered notes.
Furthermore, there is one beneficial opportunity that usually goes unnoticed, which is additional billing. Some patients require more than the initial 20 minutes of care, which makes them eligible for add-on billing under CPT 99458. By early identifying these patients, you can use better RPM reimbursement strategies and ensure that the extra time spent on care is properly reimbursed.
However, to work this consistently, standardization across your care team is important. The chances of missed billing opportunities are reduced when everyone follows the same process of documenting and tracking time. This improves accuracy as well as strengthens overall RPM billing optimization.
Strengthen Documentation for Audit-Proof Reimbursement
As your RPM workflows become more structured, documentation becomes the backbone of your ability to maximize RPM reimbursement. Yet even incomplete or unclear records can also lead you to missed payments or claim denials.
To maintain detailed and accurate records of every patient interaction, factors like vitals, communication logs, and any clinical decisions made during the care process are important. Strong documentation supports better care and ensures your remote patient monitoring reimbursement is strengthened by clear evidence.
To make this more reliable, many providers are now using digital systems that can automatically generate audit trails. These systems help you to ensure that every billable activity is directly linked to a patient encounter. This accuracy level is necessary for compliant Medicare RPM reimbursement, especially during audits where every detail matters.
Generative structured monthly clinical summaries are also important, which help you to demonstrate medical necessity. For example, when your documentation highlights why care was needed and how it was delivered, it becomes much easier to justify reimbursement.
Another important pointer is regularly reviewing billing reports to identify denied claims or recurring coding errors early. Rather than reacting after losing your revenue, this proactive approach helps you to strengthen your RPM reimbursement strategies over time.
Audit-ready documentation not only ensures compliance but also creates consistency. When your records are complete, accurate, and easy to track, you can reduce the risk of denials while building a more stable and predictable revenue stream via effective RPM billing optimization.
Workflow Optimization Strategies to Maximize RPM Reimbursement
As your program scales, managing everything efficiently becomes as important as care delivery. Without clear workflows, it’s harder to maximize RPM reimbursement consistently.
This makes it necessary to standardize your care team’s work. As we discussed earlier, when everyone is on the same page and following the same process, it becomes much easier to track activities and support accurate remote patient monitoring reimbursement.
With this, a reduction in unnecessary manual work can also make a big difference. Aligning your clinical and billing teams reduces the chances of missing details, making your overall RPM reimbursement strategies more effective.
Furthermore, it also helps you to focus more on patients who need more regular monitoring. These patients tend to stay more engaged, which further supports better results, helping you to understand how to increase remote patient monitoring revenue.
In some cases, combining RPM with CCM can improve reimbursement when done correctly. Lastly, simple and well-connected workflows make it easier to stay consistent, enhance efficiency, and achieve better RPM billing optimization.
Leveraging AI & Technology for RPM Billing Optimization

The next step after well-structuring your workflows is using the right technology to support them. It becomes difficult for you to consistently maximize RPM reimbursement without the right tools.
Thus, the RPM platforms are important, as they bring clinical, operational, and billing activities into one system. This makes it easier for them to manage remote patient monitoring reimbursement without depending on multiple tools or manual tracking.
One of the biggest advantages of it is AI-based time tracking and automated documentation. Rather than relying on manual entries, these systems can capture clinical activities in real-time. This helps you to reduce errors and ensures that all billable time is recorded accurately.
The real-time approach makes it easier to stay compliant with Medicare RPM reimbursement guidelines. For example, whether it’s meeting the 16-day device usage requirement or completing the 20-minute criteria for care management.
By reducing manual work and enhancing visibility, automation helps you to minimize missed billing opportunities. This helps you to strengthen your RPM reimbursement strategies, ensuring more consistent outcomes.
Common Mistakes That Reduce RPM Reimbursement
As we discussed above, even one small gap can make it difficult for you to maximize RPM reimbursement. Let’s take a look at some common mistakes that can lead you to miss revenue:
| Mistake | Impact on Reimbursement |
|---|---|
| Missing time tracking or incomplete documentation | Leads to underreported services and reduced remote patient monitoring reimbursement |
| Incorrect CPT code usage | Causes claim denials or delays in Medicare RPM reimbursement |
| Failure to meet CMS requirements (16-day or time thresholds) | Results in missed billing cycles entirely |
| Low patient adherence | Limits the ability to apply effective RPM reimbursement strategies |
| Lack of workflow standardization | Creates inconsistencies and affects overall RPM billing optimization |
Conclusion
Successful RPM relies on engaged patients, accurate tracking, thorough documentation, and clear workflows. When all these elements work together, it becomes easier to maximize RPM reimbursement while maintaining consistent remote patient monitoring reimbursement.
Additionally, combining structured processes with automation is what drives better results and stronger RPM billing optimization.
With integrated solutions like eCareMD, you can ensure that no billable activity is missed and stay aligned with Medicare RPM reimbursement requirements. Click here to learn more about how eCareMD ensures no billable time is missed and helps you maximize RPM reimbursement effortlessly.