Ever wondered why, despite the strong revenue potential of RPM, many practices still struggle to capture it fully?
Well, Remote Patient Monitoring (RPM) sounds simple on the surface, like monitoring patients remotely, tracking their data, and getting reimbursed for the provided care. However, things get difficult once you start billing for it.
Many practices are still experiencing denied claims, delayed payments, or confusion around what actually qualifies for reimbursement. The reason is not that they’re doing something wrong, but rather that RPM billing requirements are much more detailed than anticipated.
Today, RPM is used extensively for managing chronic conditions and enhancing patient engagement, while becoming a promising way to generate recurring revenue. However, wider adoption demands better accuracy.
Payers are paying more attention to how services are documented, how time is tracked, and whether providers are fully aligned with remote patient monitoring billing requirements.
This is where gaps begin, especially in documentation detail, time tracking, and proper alignment with billing requirements.
With evolving RPM billing guidelines and strict RPM documentation requirements, implementing a clear, structured approach is essential.
Anyhow, once you understand what really matters, RPM billing becomes much easier to manage.
In this blog, let’s explore 8 essential rules for RPM billing and reimbursement, which help you to follow CMS guidelines for remote patient monitoring claims.
So, without further ado, let’s get started!
Rule 1: Documenting Medical Necessity, Established Patient Status & Consent
Before you think about codes, claims, or reimbursement, everything in RPM billing starts with one foundation – Proper Documentation.
In many cases, claims are denied because documentation doesn’t clearly justify the billed service. This is why understanding RPM billing requirements at the eligibility level is very important.
Let’s start with medical necessity. Your RPM should always be linked to a documented condition such as hypertension or diabetes. If you don’t clearly mention this connection in your patient record, the claim may not meet the remote patient monitoring billing requirements.
Another important aspect is patient status and consent. Before starting RPM, Medicare requires that providers have an established relationship with the patient and properly document their consent.
This includes co-pay acknowledgment, whether the consent is given verbally or in writing. Missing any of these steps can lead to issues during billing or audits.
Additionally, you should make sure that the patient’s consent is timestamped. This helps you to stay audit-ready and aligned with CMS guidelines for remote patient monitoring claims.
At this stage, be sure to check for missing notes, unclear consent, and incomplete patient details. As they are minor mistakes, but together they can disrupt your claims and lead to avoidable denials.
Rule 2: Utilizing FDA-Defined Medical Devices (CPT 99453, 99454)
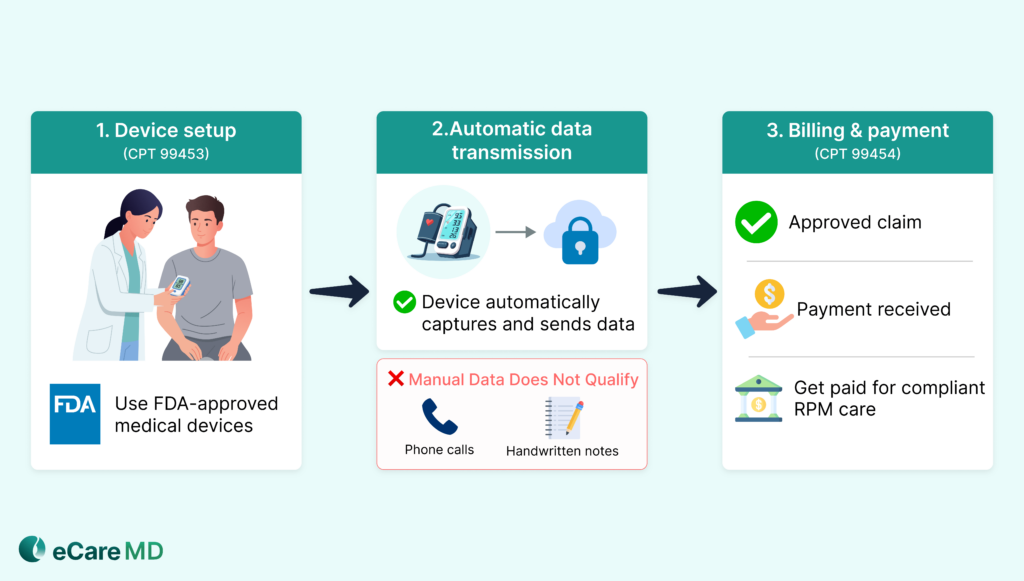
After proper documentation, the next important step is making sure that the data you’re billing for is coming from the right source.
Under RPM billing requirements, CMS clearly stated that your data must be collected by using FDA-approved medical devices. Manually reported data does not qualify for billing under CPT 99453 and 99454, as these codes require data to be automatically collected and transmitted by an RPM device, although such data may still support clinical decision-making. For example, manually reported readings, like a patient calling in their numbers or writing them down, don’t qualify for billing.
Because of these requirements, it is essential to understand how these CPT codes function and what is expected when applying them in practice:
1. CPT 99453 – Initial setup & patient onboarding:
Covers the one-time process of setting up the RPM device and educating the patient on its proper use, ensuring they are equipped to begin monitoring correctly from the start.
2. CPT 99454 – Ongoing device supply & data transmission:
Used for the continued provision of the RPM device, including the collection and automatic transmission of physiological data over a defined monitoring period.
3. Strict requirement for automated data capture:
Both codes rely on devices that automatically record and transmit patient data, eliminating eligibility for manually entered or self-reported readings.
4. Compliance goes beyond device distribution:
Billing these codes is not just about providing a device—it also requires ensuring the device meets regulatory standards and is consistently used as intended for accurate data capture.
5. Documentation and usage consistency matter:
Proper records must support that the device is actively used and transmitting data as required, as gaps can lead to denials or audit risks.
This is where confusion often arises, particularly when distinguishing between medical-grade devices and consumer wearables. Since not all devices meet RPM billing standards, using non-qualified devices can put your claims at significant risk.
The difference between medical-grade devices and consumer wearables is a common point of confusion. As not all devices can qualify, non-qualified devices can put your claims at high risk.
For instance, Many consumer wearables like fitness trackers and smartwatches do not qualify unless they are FDA-defined and capable of compliant data transmission.
The next important requirement is automatic data transmission. Without relying on manual input, the device should be able to transmit patient data electronically, meeting remote patient monitoring billing requirements. This ensures accuracy, consistency, and compliance with Medicare RPM billing standards.
Here you might be wondering about: ‘Where do practices usually run into trouble?’
Well, the answer is using non-compliant devices, relying on manually reported data, or not fully understanding device eligibility are some of the common issues. These issues can ultimately lead to claim denials and disrupt the reimbursement process.
The key to overcoming these issues is ensuring that your devices meet all requirements. This also helps you to create a reliable data flow, which can further support accurate and consistent reimbursement.
Rule 3: The 16-Day Data Transmission Requirement (CPT 99454)
Using the right device is only one part of the whole process; the next important thing is how consistently it’s used.
Under RPM billing requirements, if the device records and transmits patient data for at least 16 days within a 30-day period, at that time, only CPT 99454 can be billed. However, if the 16-day requirement is not met, CPT 99454 cannot be billed for that period.
- 16-day minimum requirement:
Device must record and transmit data on at least 16 days within a 30-day cycle
- Billing dependency:
Failure to meet this threshold makes the code ineligible for reimbursement.
So what actually counts as valid data?
To align with remote patient monitoring billing requirements, the data you collect must be physiological, such as blood pressure, glucose levels, or weight. Additionally, data must be transmitted automatically through the device.
- Type of data required:
Must be physiological (e.g., blood pressure, glucose, weight)
- Mode of transmission:
Data must be automatically captured and transmitted, manual entry does not qualify.
Yet, irregular readings or gaps in transmission can affect eligibility for billing. This is exactly where patient adherence becomes important.
If your patients are not using the device regularly, you may fall short of the 16-day requirement. In most cases, practices realized this at the end of the billing cycle, when it’s already too late to recover.
That’s why many providers are shifting towards proactive monitoring. Simple steps, including tracking daily usage, setting reminders, or using automated alerts, can assist you in ensuring that your patients stay on track throughout the month. This proactive approach helps you to enhance engagement while helping you to stay aligned with Medicare RPM billing expectations.
Rule 4: Meeting the 20-Minute Clinical Monitoring Requirement (CPT 99457 & 99458)

The next step is documenting the total time you spend acting on it. CPT 99457 covers at least 20 minutes of clinical monitoring and management within a calendar month. And if your care team spends additional time beyond that, CPT 99458 can be used for each extra 20-minute.
But what actually counts as billable time?
To align with remote patient monitoring billing requirements, this time should include meaningful clinical work. These include reviewing patient data, communicating with patients, adjusting care plans, and coordinating care when needed.
It’s not just collecting data, but actively using that data to manage your patient’s condition. This is where many practices face challenges. A substantial amount of clinical work takes place monthly, yet much of it goes untracked. Small interactions like quick patient calls or brief data reviews are usually missed or not documented in real time.
As a result, you may meet the requirements but still fall short on billing. To avoid this, accurate time tracking becomes essential. Many practices are now utilizing automated tools to log interactions and monitor time, which assist them in staying aligned with Medicare RPM billing expectations.
Rule 5: Establishing Monthly Interactive Communication
Along with time tracking, meaningful patient interaction is also necessary. CPT 99457 needs at least one real-time (synchronous) interaction with the patient each month. Without this, the service you provided may not qualify for billing.
This interaction must be live and directly involve the patient to meet the remote patient monitoring billing requirements. Additionally, it should be properly documented and connected to the care being provided.
Here’s what compliant communication typically looks like:
| Requirement | What It Means for Your Practice |
|---|---|
| Synchronous interaction | Real-time communication, not delayed or passive |
| Accepted formats | Real-time audio (phone calls) or audio-video (telehealth/video consultations) communication |
| Clinical relevance | Discussion should relate to patient data or care plan |
| Documentation | Record the interaction and link it to care decisions |
Consistency in communication improves both clinical outcomes and billing reliability. But, even after real-time communication, gaps often occur in how well it’s documented. Missing details or a lack of connection to clinical decisions can affect compliance with RPM documentation requirements.
While consistent communication and clear documentation can strengthen your overall Medicare RPM billing process and support accurate reimbursement.
Rule 6: Adhering to General Supervision Guidelines
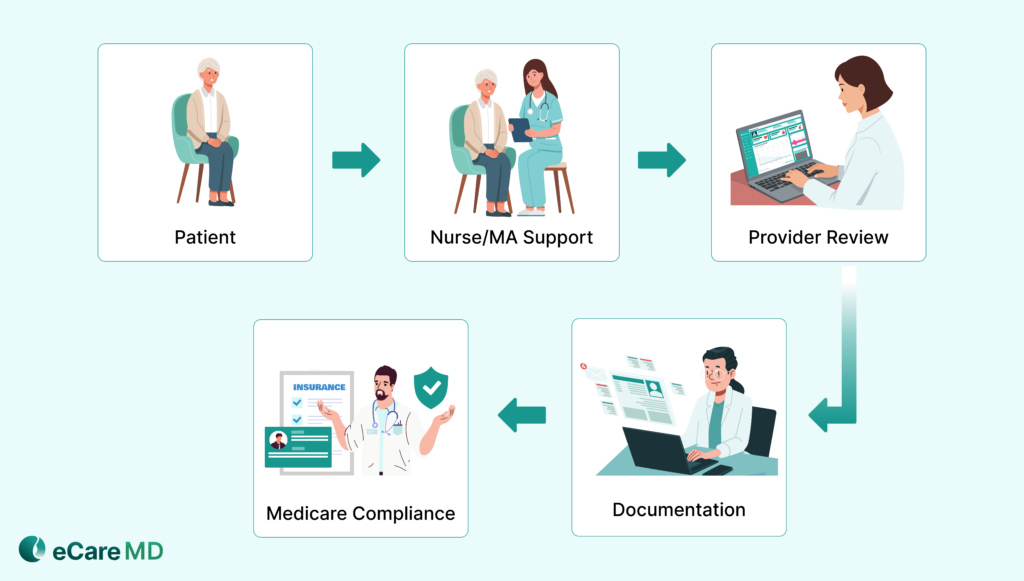
Under RPM billing requirements, your clinical staff, like nurses (RNs) or medical assistants (MAs), can also deliver services under general supervision. It means that the billing provider doesn’t have to be physically present, but they should oversee the care being delivered.
This setup allows you to scale RPM efficiently and stay aligned with RPM billing requirements. However, the billing provider remains accountable for the service. They are expected to review the patients’ data, stay informed about the care being provided, and ensure everything meets Medicare RPM billing standards.
Even so, as multiple team members are involved, there are chances of compliance issues. That’s why having a structured workflow is important. Clear role assignment, regular provider review, and proper documentation are some of the key factors that can help you ensure that every service is supervised appropriately.
Rule 7: Maintaining RPM Documentation Requirements for Audit Readiness
By this step, you may be delivering the right care by using the right devices and tracking time correctly, but if your documentation doesn’t support it, none of it matters. Documentation is something that always validates every service you bill.
It involves recording information while making sure that every part of your RPM workflow is clearly captured and easy to verify.
Let’s have a look at the table, which involves some of the key elements that your records should consistently include:
| Documentation Element | What to Capture |
|---|---|
| Device data logs | Patient readings collected through RPM devices |
| Timestamps | Dates and times of data transmission and interactions |
| Clinical time records | Time spent on monitoring, review, and care management |
| Patient communication | Details of calls or video interactions |
| Consent & eligibility | Proof of patient consent and established relationship |
Each of these elements must directly support the CPT codes you’re billing. Any gaps, like missing timestamps or incomplete tags, can create issues with Medicare RPM billing and delay reimbursement.
However, keeping all this information accurate and organized can be difficult if you do it manually. If you miss any details or scatter any records, it becomes difficult for you to prove that all RPM billing requirements were met.
To simplify this, many practices are using automation and AI, which can track data, log time, and organize documentation in one place. Additionally, it can reduce errors and make your records audit-ready without adding extra work.
Rule 8: Verifying Payer-Specific Billing Nuances & Claim Rules
Even when everything is done right, like documentation, devices, time tracking, and communication, claims can still get denied if payer rules are not followed. Commercial payers may follow different rules from Medicare RPM billing guidelines. Still, many practices face issues assuming that all payers work the same way.
To avoid this, one key point to remember is the one-provider-per-patient rule within a 30-day cycle. In many cases, only one provider can bill RPM services for a patient during that time.If you don’t check this, it can lead you to claim rejections.
That’s why it is necessary to review payer-specific RPM billing guidelines before submitting any claim. It also helps you to do a quick final check before submission. Additionally, documentation verification, confirming time requirements, and duplicate billing checking also help you to prevent common errors.
Conclusion
RPM billing works best when every step is done right, from documentation and device compliance to time tracking and communication. These RPM billing requirements are all connected, and even small gaps can affect reimbursement.
When you follow clear RPM billing guidelines, maintain proper RPM documentation requirements, and verify payer rules, your billing becomes more accurate and predictable.
With the right support, this becomes even easier. At eCareMD, practices streamline their RPM workflows, automate documentation, and stay aligned with compliance requirements, helping them reduce denials and achieve consistent reimbursement with less manual effort.